Knowing what to expect from chemotherapy treatment can help you feel more in control.
What is chemotherapy?
Chemotherapy or "chemo" uses drugs to kill cancer cells while doing the least possible damage to normal cells.
Depending on the type of cancer you have, chemotherapy may be the only treatment you need.
Before any treatment begins, make sure that you have discussed and understood your treatment team's advice. You may ask for a second opinion if you want one.
Cancer is a disease of the body's cells. It starts in our genes. Our bodies are constantly making new cells, a process controlled by certain genes. Cancers are caused by damage to these genes. As the damaged cells replicate a lump or tumour is formed.
Tumours can be:
- Benign - not cancerous. These do not spread to other parts of the body.
- Malignant - cancerous
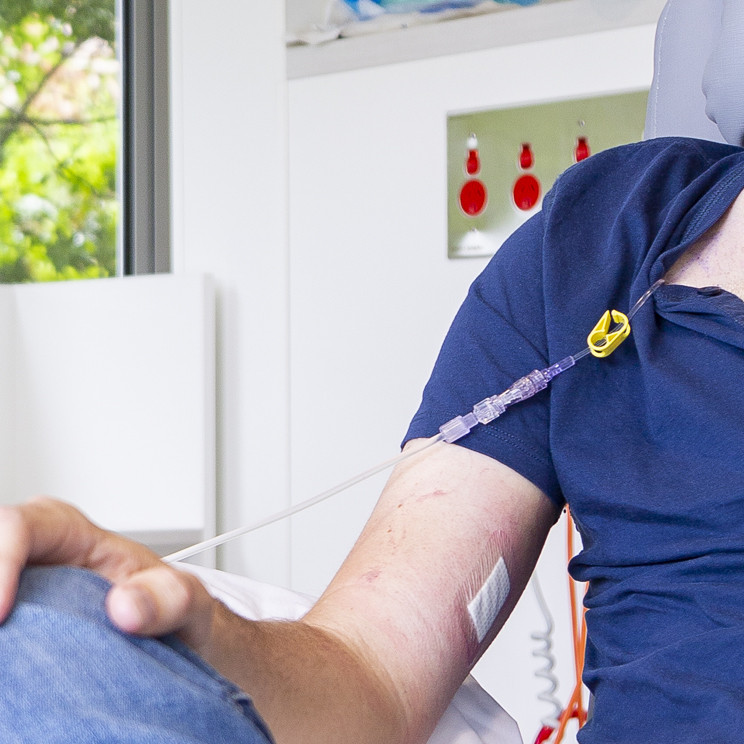
How chemotherapy works
Chemotherapy travels through the bloodstream to stop or slow the growth of rapidly dividing cancer cells.
Cancer cells exposed to chemotherapy medication are less likely to grow back than non-treated cancer cells.
Chemotherapy also affects healthy cells. The effects of chemotherapy on healthy cells cause the side effects people experience. Healthy cells can grow again.
When is chemotherapy used?
Chemotherapy can be used to:
- cure your cancer
- shrink the cancer before an operation
- help radiation treatment to work more effectively
- relieve some of the symptoms caused by your cancer
- reduce the possibility of your cancer coming back
- help you live longer
Your treatment team will offer the best treatment for you based on the type and stage of cancer as well as your general health.
This means you may have different treatments from someone else, even if their cancer type is the same type as yours.
Before any treatment begins, make sure that you have discussed and understood your treatment team's advice. You may ask for a second opinion if you want one.
Side effects of chemotherapy
Chemotherapy can also damage fast-growing healthy cells.
This damage to healthy cells is what causes side-effects during chemotherapy treatment. Most side-effects should go within a few weeks, while others can last longer.
Side effects include:
- hair loss
- forgetfulness or "chemo brain"
- numbness, tingling and hearing changes
- hot flushes and early menopause
- infertility
- feeling sick and vomiting
- itchy skin and other skin problems
Some side-effects of chemotherapy can be very serious:
- fever – a temperature over 38˚C
- chills – shivers or shakes, feeling hot or cold
- vomiting that continues after taking anti-sickness medication
- diarrhoea – four or more loose bowel movements than usual and/or diarrhoea
- gum or nose bleeds, or unusual bleeding (if bleeding does not stop after 10 minutes of ice and pressure)
- burning or blood when you pee
- chest pain
- difficulty breathing
You must contact your treatment team or go to your nearest hospital emergency department immediately and tell them you are receiving chemotherapy treatment.
Using other medications or treatment
Chemotherapy can mix with common medicines and cause harmful side-effects.
People with cancer might also think about using complementary therapies or traditional healing.
It is important to let your treatment team know about any other medicines or supplements you are taking so they can check for any known reactions.
Talk with your treatment team before having any vaccinations.
Using complementary or traditional healing
Sometimes people with cancer might think about using complementary therapies or traditional healing.
Some alternative, complementary and traditional healing methods may react with the treatment you receive and cause harmful side-effects.
It is important to talk to your treatment team about any other therapies you’re using or thinking about because they may interfere with hospital treatment.
We know that going through cancer is tough and can raise many questions. You are not alone.
We have health professionals to answer your questions and provide the support you need.
Get in touch


